Last Updated on November 28, 2025
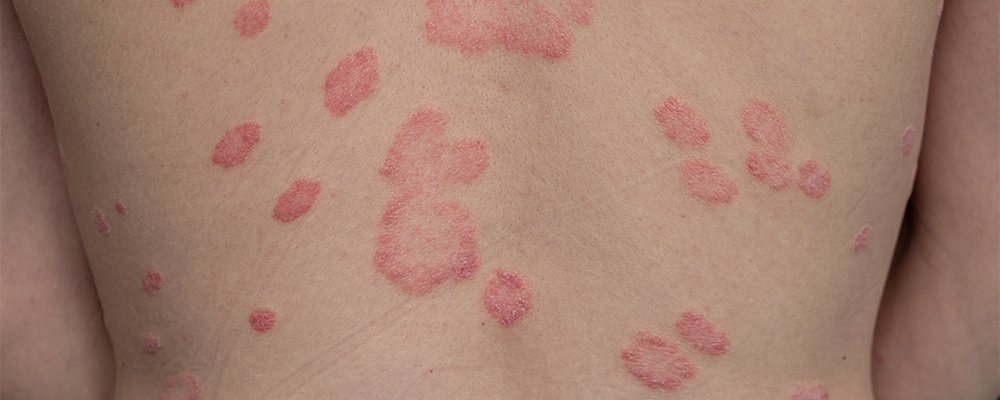
Signs and Symptoms of Tumid Lupus
Tumid lupus presents with distinctive skin changes that can help in early recognition and diagnosis of the condition.
- Causes red, swollen patches (plaques) on the skin that don’t have ulcers or scaling.
- Unlike discoid lupus, it does not cause scarring, thinning of skin, or plugged hair follicles.
- Usually affects sun-exposed areas like:
- Face
- Upper chest (V-neck area)
- Upper back
- Outer arms and shoulders
- Rarely, it can appear on the legs.
- Most cases appear during the summer months in temperate climates.
- The patches can sometimes form a ring-like (annular) pattern, similar to another type called SCLE, but with less swelling in the center.
- Less common signs include:
- Following Blaschko’s lines
- Scalp involvement that may look like alopecia areata
- Swelling around the eyes
Cause of Tumid Lupus
The exact cause of tumid lupus is not fully understood, but several factors may contribute to its development:
Genetic Predisposition:
1- Some people may have a family history of autoimmune conditions, which can make them more likely to develop tumid lupus.
2- Certain genes may influence how the immune system responds to triggers like sunlight or infections.
Immune System Dysfunction:
1- Tumid lupus occurs when the immune system mistakenly attacks healthy skin tissue.
2- This abnormal immune response causes inflammation, leading to the red, swollen patches seen in affected areas.
Sun Exposure:
1- Ultraviolet (UV) light from the sun can trigger or worsen skin lesions in tumid lupus.
2- Sun-exposed areas such as the face, chest, back, and shoulders are most commonly affected.
Environmental Triggers:
1- Some medications, infections, or other external factors may act as triggers in susceptible individuals.
2- These triggers can sometimes initiate the onset of lesions or make existing ones worse.
Essentially, tumid lupus develops from a combination of genetic susceptibility, immune system overactivity, and environmental triggers, with sunlight being a major factor.
Diagnosis of Tumid Lupus Erythematosus
Tumid lupus erythematosus (TLE) is usually diagnosed by looking at specific skin signs and tissue changes under a microscope. Other tests, like checking how the skin reacts to sunlight or seeing if antimalarial medicines help, can confirm the diagnosis but are not always needed.
Signs doctors look for:
- Skin appearance: Smooth, red, slightly raised patches on areas exposed to the sun.
- Tissue changes: Inflammation around blood vessels and skin structures, along with a jelly-like substance called mucin. The top layer of the skin is usually normal.
- Phototesgting: Lesions may appear or worsen after UVA or UVB exposure.
- Response to treatment: Quick improvement with antimalarial medications supports the diagnosis.
Treatment of Tumid Lupus Erythematosus
Effective management of tumid lupus focuses on protecting the skin, reducing inflammation, and preventing relapses. Treatment options are categorized into first-line, second-line, and third-line therapies depending on the severity and response to conservative measures.
First Line Treatments
1. Photoprotection:
Protecting affected areas from sunlight is a crucial first step. Measures include:
- Applying water-resistant sunscreen with an SPF of 30 or higher.
- Wearing protective clothing and avoiding peak sun exposure.
- Avoiding known triggers, such as smoking, to reduce the risk of lesion recurrence.
2. Topical and Intralesional Treatments:
- Topical corticosteroids are commonly applied twice daily for 2–4 weeks to reduce inflammation.
- Low-potency corticosteroids for facial lesions.
- Moderate- to high-potency corticosteroids for lesions on the torso or extremities.
- Topical calcineurin inhibitors and intralesional corticosteroids may also be used in select cases.
3. Antimalarial Medications:
- Hydroxychloroquine or chloroquine can be used for patients who do not respond adequately to topical therapies or have more extensive disease.
- Improvement may take 8–12 weeks, and studies show about 6 in 10 patients benefit from hydroxychloroquine.
4. Second-Line Therapies:
For patients with persistent or severe lesions despite first-line treatments:
- Methotrexate or mycophenolate mofetil, often combined with folic acid supplements, can be considered.
5. Third-Line and Adjunctive Treatments:
- Thalidomide or lenalidomide may be options when all previous treatments fail.
- Pulse dye laser therapy can be effective for suppressive, non-curative management of lesions.
Exploring New Treatment Possibilities for Skin Disorders
Dermatology clinical trials evaluate potential new treatments and medications for skin conditions, including inflammatory, autoimmune, and rare disorders. They help assess safety and effectiveness while giving patients access to advanced therapies under expert care.
A lupus clinical trial in Boston may test new treatment possibilities for cutaneous lupus. Participants are closely monitored and contribute to research that can improve lupus treatment options.
Conclusion:
In conclusion, tumid lupus erythematosus is a rare form of cutaneous lupus that primarily affects the skin, with lesions commonly appearing on sun-exposed areas. Early recognition of signs and symptoms, combined with proper diagnosis, is essential for effective management. Treatment focuses on protecting the skin, reducing inflammation, and preventing relapses, with options ranging from topical therapies and antimalarials to systemic medications in severe cases. Ongoing dermatology clinical trials offer hope by exploring new treatment possibilities for cutaneous lupus, allowing patients to access potential new treatments while contributing to research that may improve outcomes for those living with this condition.
Need support for your clinical trials?
Your journey to better care starts here, reach out to us today!
